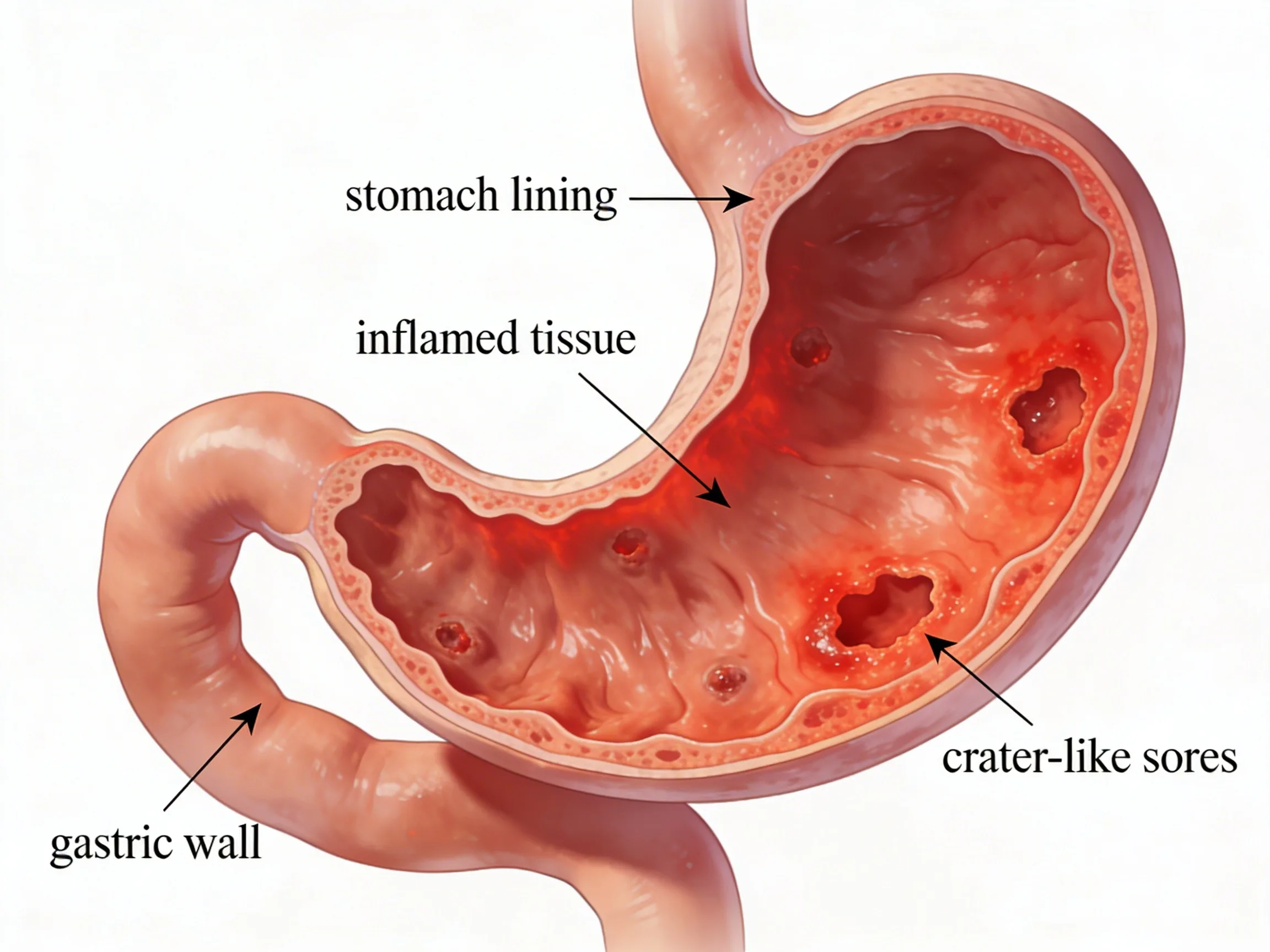
Ulcers are among the most prevalent digestive disorders globally, affecting millions across every age group. An ulcer — medically termed a peptic ulcer — is an open sore on the inner lining of the stomach, upper small intestine, or occasionally the lower oesophagus. When the mucous layer protecting digestive tissue from acidic juices weakens, stomach acid erodes the tissue beneath, creating a wound that can profoundly impact daily life.
Understanding what causes ulcers, recognising the early signs, and knowing which foods and treatment approaches support healing is essential for preventing complications and restoring lasting digestive wellness. This comprehensive resource covers everything from stomach ulcer symptoms to peptic ulcer causes, the best diet for ulcer patients, and how holistic treatment philosophies may complement your recovery journey.
Untreated ulcers can lead to internal bleeding, perforation (a hole through the stomach wall), or gastric outlet obstruction. Identifying the early signs of a stomach ulcer and consulting a professional promptly can prevent these serious outcomes and significantly improve quality of life.
What Are Ulcers?
An ulcer is an erosion or open sore that forms when the protective mucous membrane lining the digestive organs is damaged, allowing stomach acid and digestive enzymes — particularly pepsin — to irritate and eat into the underlying tissue. The term "peptic ulcer" is the umbrella medical name for these sores, derived from "pepsin," one of the key digestive enzymes involved.
Peptic ulcers are classified by location:
- Gastric ulcers — sores on the stomach lining itself
- Duodenal ulcers — sores in the upper small intestine (duodenum); the most common type
- Oesophageal ulcers — less common sores in the lower oesophagus, often linked to chronic acid reflux
Under normal conditions, a thick mucus layer shields the stomach lining from hydrochloric acid (pH 1.5–3.5 — strong enough to dissolve metal). When this delicate balance is disrupted — by bacterial infection, certain medications, or other factors — acid gains access to sensitive tissue, and an ulcer develops.
Peptic ulcer disease affects approximately 5–10% of the global population at some point. Duodenal ulcers are roughly four times more prevalent than gastric ulcers. In India, prevalence is notably higher in southern and eastern regions, with dietary patterns and H. pylori infection rates as contributing factors.
Early Signs and Symptoms of Ulcers
Recognising stomach ulcer symptoms early is crucial. Symptoms range from mild discomfort to severe pain and vary between gastric and duodenal ulcers. Some individuals — particularly older adults or those on NSAIDs — may have "silent" ulcers with minimal symptoms until complications occur.
Common Ulcer Symptoms in Adults
Burning Stomach Pain
The hallmark symptom — a burning, gnawing, or hunger-like pain in the upper abdomen between the breastbone and navel. Worsens on an empty stomach, between meals, or at night.
Bloating & Fullness
Persistent feeling of fullness, abdominal distension, or uncomfortable bloating — even after eating small amounts. Frequent belching is also common.
Nausea & Vomiting
Frequent nausea during or after eating. In severe cases, vomiting with traces of blood (bright red or dark coffee-ground material) may indicate a complicated ulcer.
Loss of Appetite
Many patients avoid eating because of post-meal pain, leading to reduced calorie intake, nutritional deficiencies, and gradual unintended weight loss.
Heartburn & Reflux
A burning sensation rising from the stomach into the chest or throat. Often worsened by lying down, bending over, or consuming acidic and spicy foods.
Food Intolerance
Increased discomfort, nausea, or pain after consuming fatty, fried, or heavy meals — a frequently reported symptom prompting medical consultation.
Ulcer Pain After Eating — Timing Matters
Gastric ulcer pain often begins shortly after eating (30–60 minutes), as food triggers acid production. Duodenal ulcer pain typically appears 2–3 hours after meals or at night when the stomach is empty, and is often temporarily relieved by eating. This cycle — pain → eating → relief → pain returns — is a key diagnostic clue.
Symptoms in Females vs Males
Stomach ulcer symptoms in females more frequently include nausea, bloating, and diffuse discomfort. Symptoms in males often present as the classic burning epigastric pain. Women face higher NSAID-related ulcer risk due to greater painkiller use for menstrual cramps and headaches.
Warning signs: vomiting blood (bright red or coffee-ground material), black or tarry stools, sudden severe abdominal pain, dizziness or fainting, and rapid heartbeat. These require immediate medical attention — do not delay.
Common Causes of Ulcers
Understanding what causes stomach ulcers is vital for prevention and effective care. Contrary to popular belief, spicy food and emotional stress don't directly cause ulcers — research has identified two primary culprits along with several contributing factors.
H. pylori Infection
Helicobacter pylori weakens the protective mucous coating. Responsible for ~60–70% of gastric ulcers and up to 90% of duodenal ulcers. Spreads through contaminated food, water, or contact.
NSAID Overuse
Aspirin, ibuprofen, naproxen, diclofenac — these inhibit prostaglandins that maintain the stomach's protective lining. Prolonged use significantly raises risk, especially in older adults.
Stress & Lifestyle
Chronic stress increases acid production and promotes unhealthy habits. Severe physiological stress from illness or surgery can cause acute stress ulcers in hospitalised patients.
Alcohol & Smoking
Alcohol erodes the stomach lining and increases acid. Smoking reduces blood flow, impairs healing, and makes H. pylori harder to eradicate. Together they dramatically elevate risk.
Genetic Factors
Family history is a recognised risk factor. Some people inherit higher acid production or thinner protective mucous layers, increasing vulnerability to ulcer formation.
Other Conditions
Zollinger-Ellison syndrome, Crohn's disease, liver cirrhosis, kidney disease, and abdominal radiation — all can damage the stomach lining and contribute to ulcer development.
Myth: "Spicy food causes ulcers." Fact: Spicy food doesn't cause ulcers but can worsen symptoms. The actual causes are H. pylori infection and NSAID overuse. Stress aggravates ulcers but isn't a direct cause on its own.
Types of Ulcers
Understanding the difference between gastric and peptic ulcers — and where duodenal ulcers fit in — helps you communicate more effectively with your healthcare provider.
Stomach Lining Ulcer
- Location Stomach lining
- Prevalence Less common
- Pain timing 30–60 min after eating
- Food effect Pain often worsens
- Age group More common over 50
- Weight Weight loss common
- Healing 6–8 weeks typically
Small Intestine Ulcer
- Location Upper small intestine
- Prevalence 4× more common
- Pain timing 2–3 hrs after eating; night
- Food effect Temporarily relieves pain
- Age group Ages 25–50
- Weight May stay stable or increase
- Healing 4–6 weeks typically
Key takeaway: "Peptic ulcer" encompasses both gastric and duodenal ulcers. All gastric ulcers are peptic ulcers, but not all peptic ulcers are gastric ulcers.
Stomach Ulcer vs Gastritis
Gastritis is inflammation of the stomach lining without an open sore — the mucosa is irritated but not eroded through. A stomach ulcer is a deeper erosion penetrating the mucosal layer. Gastritis can precede and progress to ulcer formation if untreated. Both share overlapping causes (H. pylori, NSAIDs) but differ in severity and management. An endoscopy definitively distinguishes between them.
Ulcer Pain Location and Warning Signs
Knowing where ulcer pain occurs and what warning signs to watch for can help identify problems early. The stomach ulcer pain location varies depending on the ulcer's type, position, and severity.
Upper Central Abdomen (Epigastric)
The most common location. Burning or gnawing pain between the navel and breastbone — where most gastric and duodenal ulcer pain is felt.
Left Upper Abdomen
Gastric ulcers on the greater curvature may produce left-sided pain, sometimes confused with cardiac discomfort.
Right Upper Abdomen
Duodenal ulcers may cause right upper quadrant pain, sometimes confused with gallbladder or liver issues.
Referred Back Pain
Posterior or deep ulcers may radiate pain to the back, between shoulder blades. Sudden severe back pain may indicate a penetrating ulcer — seek immediate care.
How to Know If You Have a Stomach Ulcer
While self-diagnosis isn't recommended, these patterns suggest an ulcer rather than simple indigestion:
- Pain follows a predictable meal-related pattern
- Antacids provide temporary but repeatedly recurring relief
- Pain wakes you at night (common with duodenal ulcers)
- Symptoms persist for days or weeks, not just hours
- Unexplained weight loss or appetite changes
- Symptoms improve then relapse cyclically
Definitive diagnosis requires professional evaluation — typically an upper endoscopy, H. pylori breath or stool test, and sometimes blood tests. If symptoms persist, consult a qualified healthcare provider.
Foods to Avoid with Ulcers
Diet plays a significant role in managing ulcer symptoms and supporting healing. While food alone doesn't cause or cure ulcers, certain items can irritate the damaged lining, stimulate excess acid, and delay recovery. Knowing what not to eat with a stomach ulcer is critical.
- ✕ Spicy foods (chili, hot sauce, cayenne)
- ✕ Citrus fruits & juices (orange, lemon)
- ✕ Tomatoes & tomato-based sauces
- ✕ Coffee (regular & decaf) & strong tea
- ✕ Carbonated & fizzy beverages
- ✕ Alcohol in all forms
- ✕ Deep-fried & greasy foods
- ✕ Processed & cured meats
- ✕ Chocolate & peppermint
- ✕ Vinegar & pickled foods
- ✕ Refined sugars & pastries
- ✕ Extremely hot or cold foods
- ✓ Bananas (natural antacid properties)
- ✓ Non-citrus fruits (apples, pears, melons)
- ✓ Cooked vegetables (carrots, sweet potato)
- ✓ Whole grains (oats, brown rice, barley)
- ✓ Lean proteins (chicken, fish, tofu)
- ✓ Yoghurt & probiotic-rich foods
- ✓ Herbal teas (chamomile, liquorice)
- ✓ Honey (especially Manuka honey)
- ✓ Olive oil & healthy fats
- ✓ Cabbage & cabbage juice
- ✓ Turmeric (culinary amounts)
- ✓ Room-temperature water between meals
Instead of three large meals, aim for 5–6 smaller meals throughout the day. This maintains a steady buffer against stomach acid. Also avoid eating within 2–3 hours of bedtime to reduce night-time acid exposure.
Best Diet for Ulcer Patients
A well-planned ulcer diet plan soothes the digestive tract, minimises acid irritation, promotes tissue repair, and supports the body's natural healing. Here are the core principles and a practical daily meal plan.
Core Dietary Principles
- Prioritise fibre-rich foods — vegetables, fruits, legumes, and whole grains reduce ulcer risk and regulate digestion
- Include daily probiotics — yoghurt, kefir, buttermilk, and fermented foods maintain healthy gut flora and may inhibit H. pylori
- Choose healing foods — cabbage (vitamin U), bananas, honey, and turmeric support mucosal repair
- Stay hydrated — drink water between meals rather than during to avoid diluting digestive juices
- Consume adequate lean protein — provides amino acids for tissue repair; bake, steam, or grill instead of frying
Sample One-Day Ulcer Diet Plan
Individual dietary needs vary. This is a general framework. If you have diabetes, kidney issues, or food allergies, work with a qualified nutritionist to customise your ulcer diet plan.
Natural and Holistic Treatment for Ulcers
Many individuals seeking stomach ulcer natural treatment want approaches that address root causes — not just suppress symptoms. Integrative systems, including homeopathy, offer a complementary perspective on supporting the body's innate healing capacity.
Natural Remedies That May Support Healing
These are not replacements for professional care but may complement a comprehensive treatment plan:
Cabbage Juice
Rich in vitamin U (S-methylmethionine), traditionally used to support gastric mucosal repair and healing.
Manuka Honey
Contains antibacterial compounds (methylglyoxal) that may inhibit H. pylori and soothe the irritated lining.
Probiotics
Lactobacillus and Bifidobacterium strains help restore gut flora and strengthen mucosal barrier defence.
DGL Liquorice
Deglycyrrhizinated liquorice may stimulate protective mucus production without affecting blood pressure.
Turmeric (Curcumin)
Anti-inflammatory and antioxidant properties may support digestive health when used in culinary amounts.
Aloe Vera Juice
May soothe digestive lining and reduce irritation. Choose inner-leaf preparations without aloin.
Homeopathic Approach to Ulcer Management
Homeopathy is founded on the principle of "similia similibus curentur" (like cures like) — a highly diluted substance that produces certain symptoms in a healthy person may stimulate healing when similar symptoms are present. In ulcer care, homeopathic practitioners take an individualised, whole-person approach, considering the patient's complete symptom picture, emotional state, digestive tendencies, and constitutional factors.
Commonly discussed remedies in the context of peptic symptoms include:
⚠️ Important Disclaimer
Homeopathic remedies are listed for educational purposes only and should not be self-prescribed. Treatment should be undertaken under a qualified practitioner's guidance as a complementary approach alongside conventional medical care. Always consult a healthcare professional for diagnosis, especially for suspected bleeding or complicated ulcers.
The Integrative Advantage
Many patients find value combining conventional diagnosis with holistic support: dietary modifications, stress management (meditation, yoga, pranayama), lifestyle adjustments, and complementary therapies like homeopathy — addressing root causes rather than merely suppressing symptoms. At PDM Homeopathy Hospital, this patient-centred, integrative philosophy is at the heart of everything we do.
Struggling with Digestive Discomfort?
Our experienced practitioners can help you explore a personalised, holistic approach to ulcer care — combining dietary guidance, lifestyle support, and individualised treatment.
Prevention Tips for Ulcers
Preventing stomach ulcers — or reducing recurrence risk — involves addressing modifiable risk factors. These evidence-informed strategies protect your digestive health long-term:
Use Pain Medications Responsibly
Take NSAIDs only when necessary at the lowest effective dose. Always take with food. Discuss alternatives with your doctor for long-term pain management.
Practise Good Hygiene
H. pylori spreads through contaminated food, water, and contact. Wash hands thoroughly, drink clean water, and ensure proper food preparation and storage.
Limit or Avoid Alcohol
Excessive alcohol damages the stomach lining and stimulates acid overproduction. If you drink, do so moderately — never on an empty stomach.
Quit Smoking
Smoking impairs blood flow to the stomach, reduces mucosal defences, and interferes with healing. Quitting significantly reduces ulcer risk and recurrence.
Manage Stress Effectively
Incorporate meditation, yoga, pranayama, exercise, and adequate sleep into your routine. Chronic stress aggravates digestive vulnerability.
Eat a Balanced, Gut-Friendly Diet
Prioritise fibre, probiotics, lean proteins, and vegetables. Avoid excessive spicy, acidic, fried, and ultra-processed foods. Maintain regular meal timings.
Get H. pylori Tested
If you have persistent symptoms or family history of ulcers, ask about H. pylori testing. Early detection enables timely and effective treatment.
Don't Ignore Persistent Symptoms
If stomach pain, bloating, or indigestion lasts more than two weeks, consult a professional rather than self-medicating. Early intervention prevents complications.
When to Consult a Doctor
While mild indigestion is common and often resolves naturally, certain symptoms warrant prompt medical evaluation to prevent serious, potentially life-threatening complications.
• Vomiting blood (bright red or dark coffee-ground material)
• Black, tarry, or bloody stools (melaena)
• Sudden, severe, sharp abdominal pain that doesn't subside
• Signs of shock: rapid pulse, cold/clammy skin, fainting
• Complete inability to keep any food or fluids down
Schedule a Consultation If You Notice:
- Burning or gnawing stomach pain persisting beyond 1–2 weeks
- Pain that consistently wakes you at night
- Unintended weight loss with digestive symptoms
- Persistent nausea, bloating, or progressive appetite loss
- Antacids provide only temporary, recurring relief
- Difficulty or pain when swallowing food
- Family history of stomach ulcers or stomach cancer
- Age over 50 with new-onset digestive symptoms
- Regular NSAID use with developing stomach discomfort
Early diagnosis through endoscopy, H. pylori breath/stool tests, or blood tests enables targeted treatment and significantly reduces the risk of bleeding, perforation, or gastric obstruction.
Why Choose PDM Homeopathy Hospital
Since 2016, PDM Homeopathy Hospital has grown to 42+ branches with the trust of 400K+ patients and 310K+ YouTube subscribers. We believe lasting wellness comes from treating the whole person — not just isolated symptoms.
Holistic, Patient-Centred Philosophy
We invest time understanding your complete health picture — physical symptoms, emotional wellbeing, dietary habits, and lifestyle — to create a genuinely personalised care plan that addresses root causes, not just surface symptoms.
Experienced Team
Qualified homeopathic physicians with extensive experience in digestive disorders including ulcers, gastritis, GERD, and IBS.
Integrative Approach
We work collaboratively alongside your existing healthcare team with dietary guidance and lifestyle counselling.
Thorough Assessment
Every consultation includes detailed review of medical history, symptoms, previous treatments, and health goals.
42+ Branches — 400K+ Patients — Nationwide Trust
With locations across India and an active community of 310K+ YouTube subscribers, PDM brings accessible, quality homeopathic care to you — wherever you are. Our track record speaks to the trust patients place in our approach to digestive and overall wellness.
Ongoing Support
Regular follow-ups, treatment adjustments, and continuous nutritional and lifestyle guidance throughout your healing journey.
Take the First Step Toward Digestive Wellness
If you or a loved one is experiencing persistent ulcer symptoms, our team is here to help with personalised, holistic care.
Frequently Asked Questions About Ulcers
Quick, clear answers to the most common questions about ulcer symptoms, causes, diet, and treatment.
⚠️ Medical Disclaimer
This content is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider regarding medical conditions. Do not delay seeking advice or disregard professional recommendations based on this information. For medical emergencies, contact your local emergency services immediately.