Advanced Homeopathy Care for Allergy, Rhinitis, Asthma, Skin Allergy, Psoriasis,
Eczema, Pain & More. | Book a Consultation with PDM Homeopathy Specialists
9050077755 | No Travel, No Waiting
-
Consult PDM Doctors Online from the Comfort of Your Home | For Queries: support@pdmhomeopathy.com
Advanced Homeopathy Care for Allergy, Rhinitis, Asthma, Skin Allergy, Psoriasis,
Eczema, Pain & More. | Book a Consultation with PDM Homeopathy Specialists
9050077755 | No Travel, No Waiting
-
Consult PDM Doctors Online from the Comfort of Your Home | For Queries: support@pdmhomeopathy.com
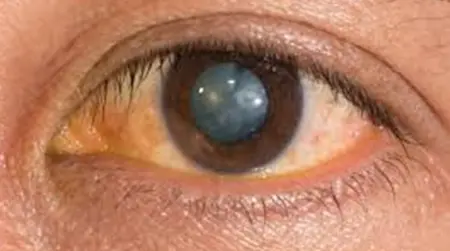
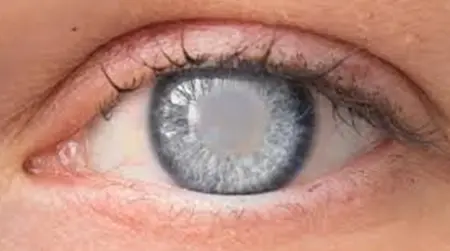
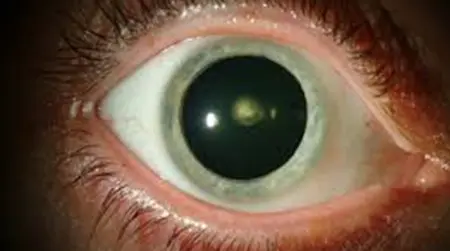
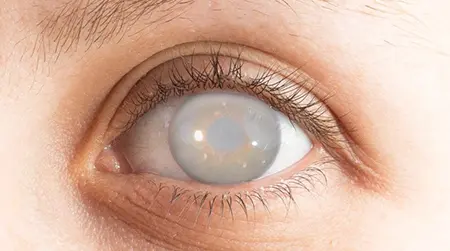
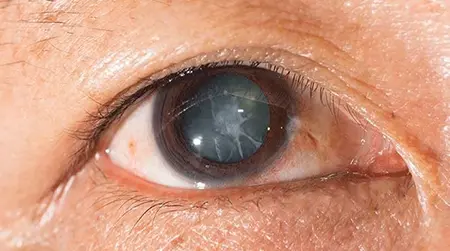
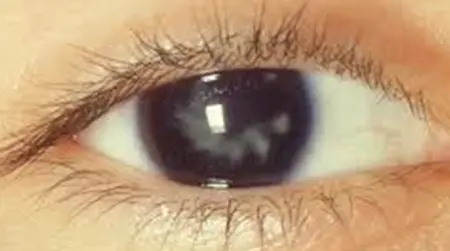
Advanced Homeopathy Treatment for Cataracts
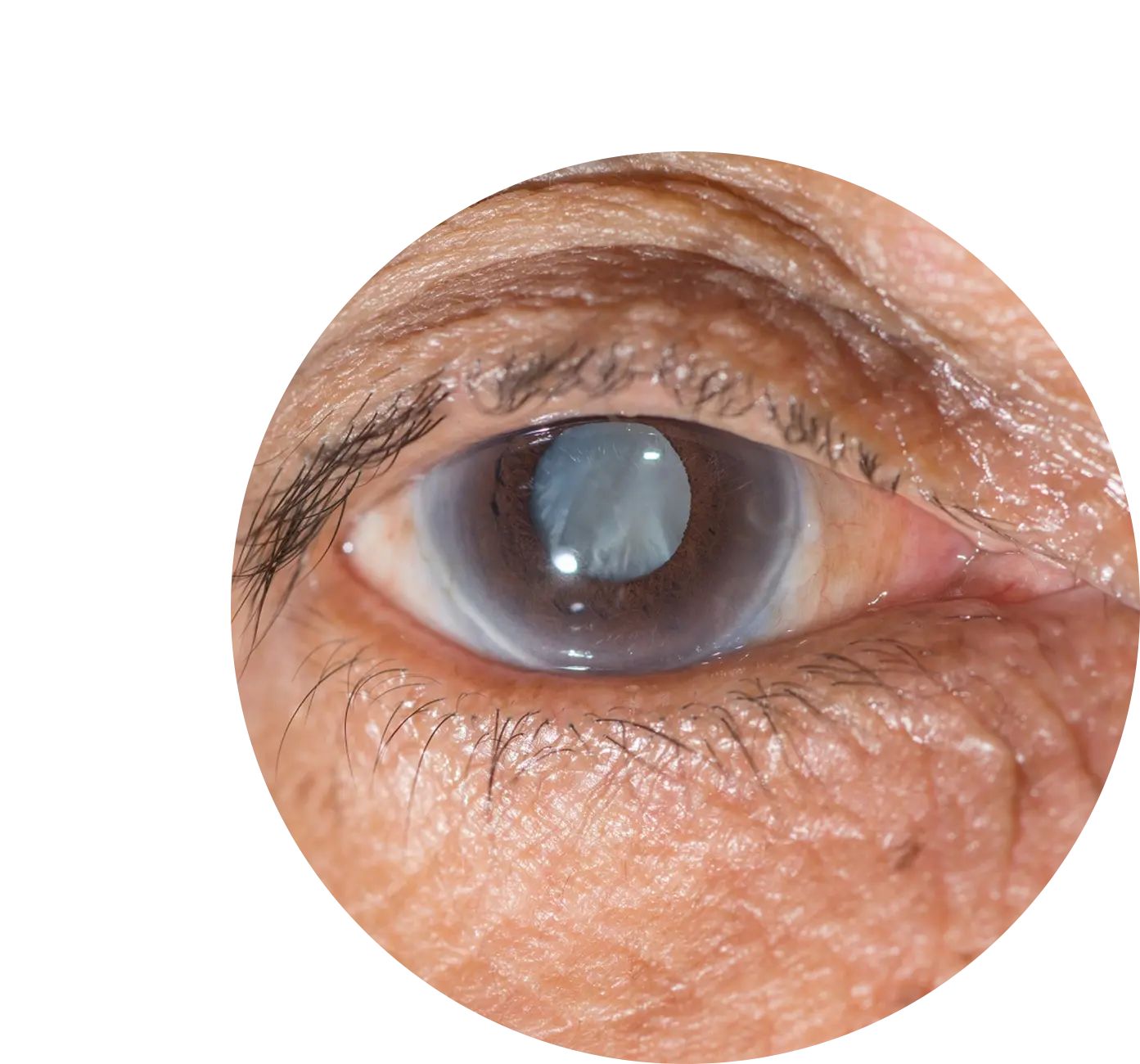
Heal your eyesight and get rid of cataracts with homoeopathic treatment at PDM Homeopathy. On average, Indians develop cataracts about 10 years earlier than people in west. Cataracts are cloudy areas on the eye lens that is naturally clear, usually caused by ageing. Early cataracts can be treated with homeopathy treatment. Our eye cataract treatment focuses on eyesight by slowing down the formation of cataracts and preventing eye lenses from being blurry, hazy, or muted in vision. Dr Ritu Choudhary (BHMS) has designed a three-phase homoeopathic treatment for a safe and long-term cure for cataracts. Experience cataracts treated in eye treatment now.
India’s Fastest-Growing Homeopathy Hospital Chain
360k+
Satisfied Patients
309k+
You Tube
140k+
42+
Branches
Cataracts have become the primary cause of blindness in India, despite being preventable. It affects nearly 66% of all blindness cases in the country. Cataracts happen due to too much sunlight exposure, nutrient deficiencies, and genetics. This starts developing in people after age 45, with a skyrocketing number of cases after the age of 65. The unfortunate part is that still 27.5% of people with cataracts have not even taken a single eye treatment in India. But our advanced homoeopathy treatment for early cataracts can prevent/pause it effectively. Since each patient is different, our homoeopathic eye doctors analyse and evaluate each cataract case individually. Other than age, rising diabetes, high blood pressure, and obesity cases are accelerating blindness more. So, it’s best to consult with a professional eye doctor of homeopathy near you.
At PDM homeopathic hospital, our eye specialists work on a three-phase treatment system designed by top homoeopathic doctor Dr. Ritu Choudhary (BHMS). We have noted that the most common issue cataract patients, especially women, face is the lack of someone to accompany them to appointments. After detailed case taking, homoeopathic medicines are planned by the eye doctor to promote long-lasting relief from cataracts and vision loss. Our advanced homoeopathic treatment offers a non-invasive and holistic approach to fix early cataracts by reducing glare and enhancing contrast for clearer vision. In case of chronic cataracts and severe situations, surgery is the only option rather than solely relying on homeopathy treatment. Our cataract treatment with homeopathy works on early cases, depending on the case. The homeopathy medicines are designed to work slowly on the body by strengthening the human constitution, not providing immediate relief.
Book a counselling call with our doctor

Dr Ritu Choudhary
- Share your health concerns
- Detailed medical history
- Know your treatment path
Detailed
Case Taking
5 mins
Quick response time
Know Your Cataracts Risk & Recovery Scope in Just 60 Seconds
Check what may be affecting your eyesight clarity. Take a quick assessment for personalised homeopathy treatment guidance.

Trusted by Patients Like You
×
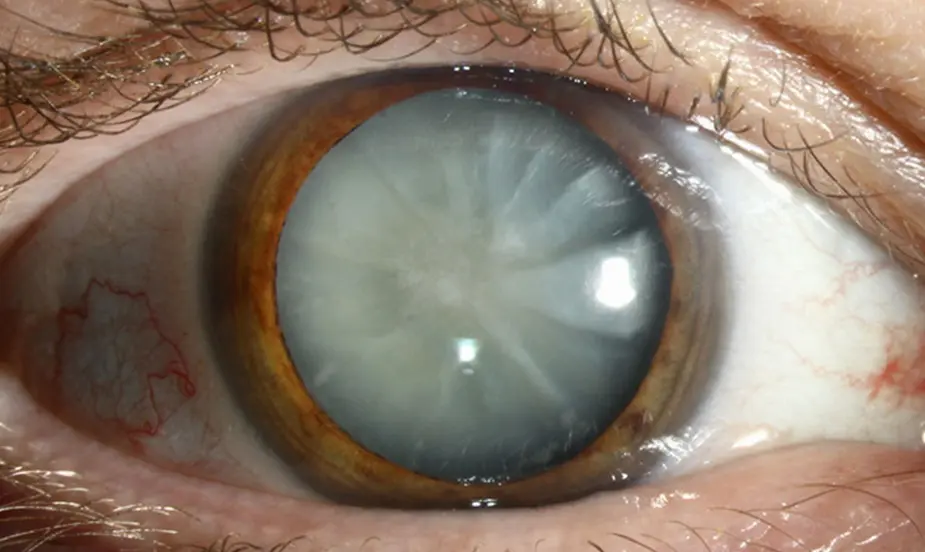
Common Triggers of Cataracts
- Bright Sunlight: Long exposure to sun rays damages eye lens slowly.
- Screen Exposure: Too much mobile or laptop use strains eyes daily.
- Smoking Habit: Smoking increases harmful changes inside eye lens.
- High Sugar: Uncontrolled diabetes speeds up cataract development in the eyes.
- Steroid Use: Long-term medicines affect lens and reduce eye clarity.
- Eye Injury: Past trauma can trigger cataract formation later.
- Poor Diet: Lack of nutrients weakens eyes and affects vision health.
- Age Changes: The natural ageing process leads to gradual lens clouding.
Cataracts Treatment: Homeopathy vs Conventional
| Treatment Feature | Homeopathy | Conventional |
|---|---|---|
| Focus on Root Cause of Cataract | ||
| Holistic Healing for Cataract | ||
| Natural Cataract Medicines | ||
| Individualised Care | ||
| Immunity Support | ||
| Long-Term Balance | ||
| Symptom Suppression |
How to Diagnose Cataracts:
To avoid eye surgery, early cataract diagnosis is very important to start treatment as early as possible. Cataract formation on the eye lens is not just due to age or common problems like diabetes, blood pressure and obesity but also long exposure to sunlight. Eye injury or certain long-term medication can also be the reason. Dr Ritu Choudhary (BHMS) always advises consulting a professional doctor who is an expert in cataract eye management for the right diagnosis. In fact, bad lifestyles, like excessive smoking and heavy alcohol intake, can trigger early cataracts even if the eyes seem okay. Our eye specialists at PDM Hospital only prescribe homoeopathic medicine that works on underlying causes instead of treating only symptoms. We test cataract issues under the supervision of a senior homoeopathic specialist of eyes and vision. Cataracts are diagnosed through a comprehensive eye exam. During an eye test, typically a doctor runs a visual acuity test, a slit-lamp examination, and a dilated retinal exam to check for lens clouding. We, as the top homoeopathic clinic, always advise patients to get proper eye test screening and start cataract treatment as early as possible. Long-term chronic cataract issues can cause complete and irreversible blindness.
Get Cataracts Relief in with Advanced Homeopathy
Consult a reputable Cataracts specialist in India and breathe easier naturally with our personalized homeopathy for Cataracts care.
Informational Videos
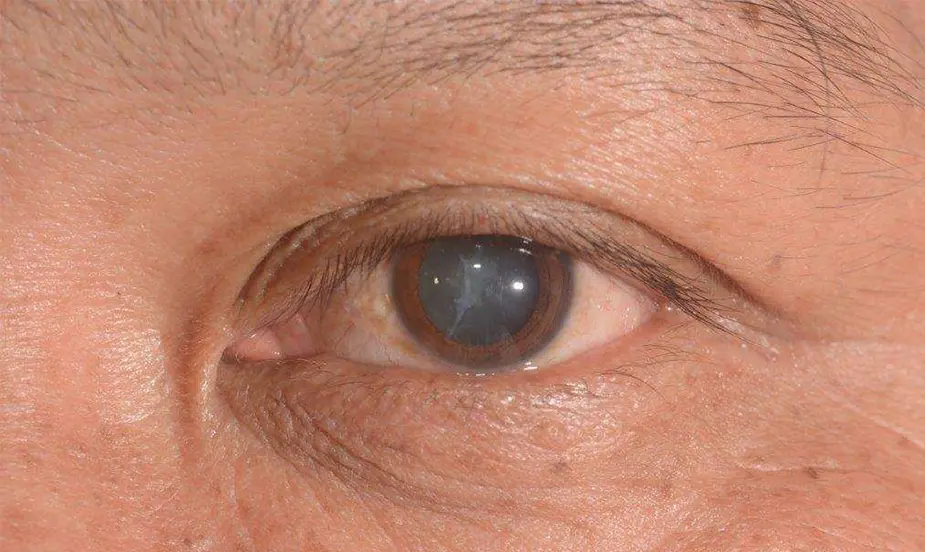
How to Prevent Cataracts?
Simple eye care habits can slow cataract formation and protect vision. Healthy lifestyle, proper nutrition, and regular eye checkups help keep eyes clear longer.
- Wear Sunglasses: Protect eyes from strong sunlight.
- Control Sugar: Keep diabetes under good control.
- Healthy Diet: Eat fruits and green vegetables.
- Quit Smoking: Smoking damages eyes and lenses.
- Limit Screen Time: Reduce long hours on screens.
- Regular Checkup: Detect early changes in eyes.
- Eye Protection: Avoid injury during risky activities.
Homeopathy Treatment Process for Cataracts
Step 1: Detailed Consultation
01.
The process begins with an in-depth discussion covering medical history, lifestyle, and condition patterns.
Step 2: Individual Assessment
02.
Each case is carefully evaluated to understand the patient’s unique health profile and disease behaviour.
Step 3: Personalized Planning
03.
Based on assessment findings, a customised homoeopathic plan is prepared and explained clearly.
Step 4: Ongoing Monitoring
04.
Regular follow-ups help track progress and adjust care as required over time.

About PDM Advanced Homeopathy
PDM Homeopathy is an advanced homoeopathic clinic established in 2016. With 10+ years of experience and 360,000+ patients treated, the clinic operated under the leadership of Dr Ritu Choudhary (BHMS). Our experienced eye doctors design personalised homoeopathic medication plans. Over 42 branches in North India, we are the #1 fastest-growing homoeopathy chain in India. With physical availability of our clinic in Rajasthan, Haryana, and Punjab, we also offer online consultation support worldwide for homoeopathic treatment. Our team of homoeopathy doctors follows a structured three-layer treatment approach that works on the root cause and heals you inside out for safer and sustainable results.
Why Choose PDM Advanced Homeopathy?
PDM Advanced Homeopathy offers protocol-based scientific treatment with personalized care. We focus on root-cause healing using safe, natural medicines and lifestyle guidance for long-term wellness.
Start Your Homeopathic Treatment for Cataracts
Frequently Asked Questions
Cataract usually does not go away on its own once it forms. In early stages, symptoms can be managed with proper care and homeopathy support. However, advanced cataracts may still require surgical removal for clear vision improvement.
Yes, cataracts can become serious if left untreated for a long time. It slowly reduces vision clarity and may lead to major vision loss. Early detection and timely care help maintain better eye function and daily comfort.
Cataracts are more common after the age of 50. However, it can develop earlier due to diabetes, injury, or long-term medicine use. Some people may notice early symptoms even in their forties.
You may notice increasing blurry vision, more glare from lights, and frequent changes in glasses numbers. Difficulty in night vision and faded colours are also signs that cataracts may be progressing.
A healthy diet rich in vitamins like A and C and antioxidants can support eye health. While it may not reverse cataracts, it helps slow down damage and keeps eyes stronger for a longer time.
Homeopathy may help in early stages by supporting overall eye health and slowing progression. It focuses on improving internal balance and reducing risk factors, but proper evaluation is needed to plan the right treatment approach.